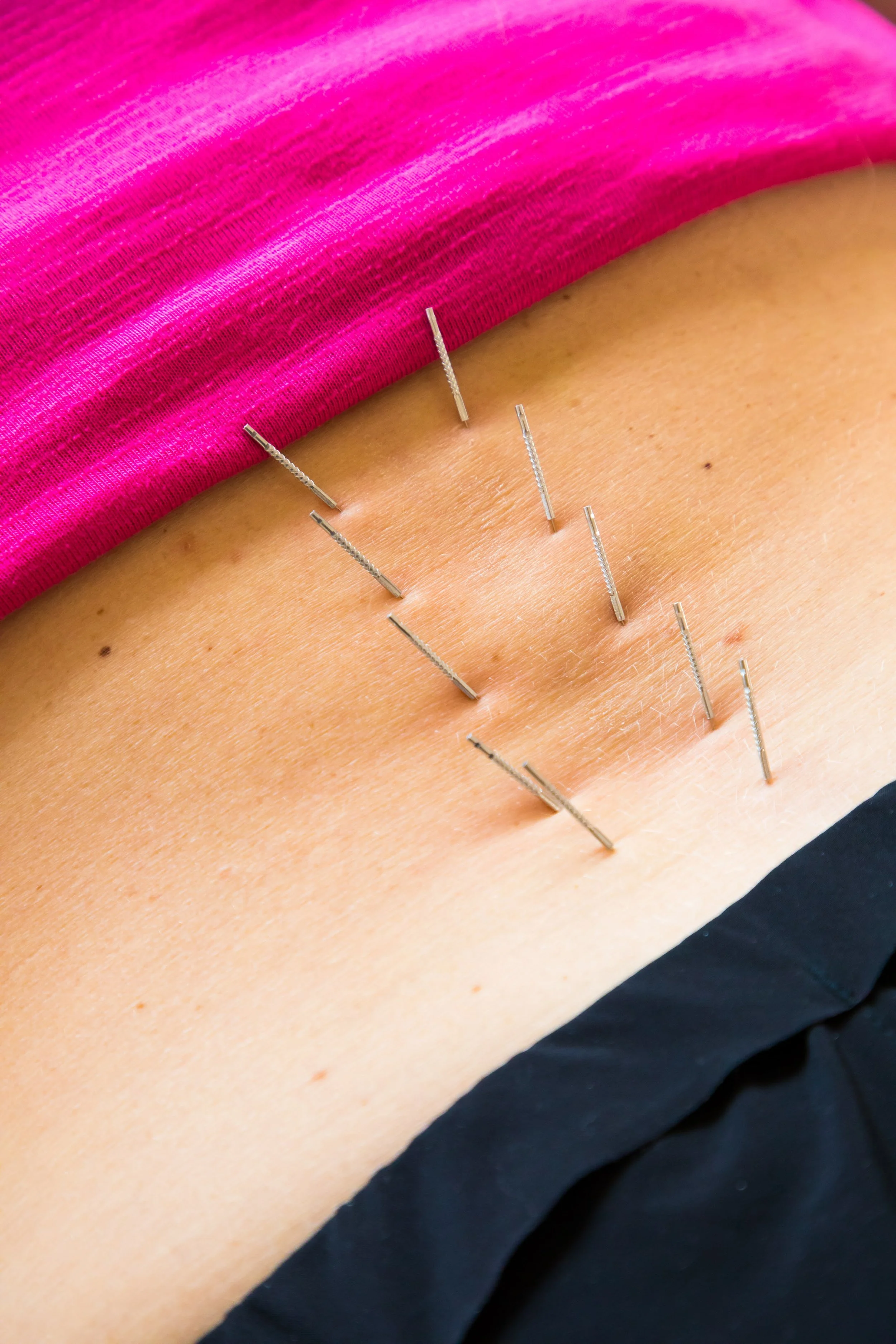
Dry Needling your back for pain, isn’t just about your back
A person walks into a clinic, after they strained their back last week with ongoing pain. They have tried all the tricks on their own to relieve it: heat, ice, stretching, pain patches; but nothing makes it better. They are offered dry needling, and they start to have some relief, and they start to feel better.
On the surface, the assumption is the needles went into the tight muscles, the muscles relaxed, and the pain went away. But in actuality it's much more interesting than that. Dry needling is not just about a localized treatment to the back. Those needles going into the back are impacting that area, but they are also influencing the entire nervous system.
Once you understand why dry needling works on the local level, you then can also understand why that matters in the long term.
Pain is complex:
Most people just understand the local level influence:
Needle goes into a tight muscle → the muscle relaxes → pain goes away
While this does occur at the specific sight of entry, this is an incomplete understanding of the process. Pain is not just a tissue or biological problem. This is especially true for pain that has been persistent or recurring pain that just doesn’t fully go away.
Pain is an output of the brain/nervous system, and not an input from the body. Our pain is not just an interpretation of what was hurt, but also layers with psychological and sociological aspects surrounding that experience on top of the biological (biopsychosocial). That’s why it’s often referred to as multifactorial experience and only treating the biological or tissue side sometimes doesn't help.
Nervous System Basics:
Our Nervous system is made up of 2 different parts:
Central nervous system (CNS) which is made up of our brain and spinal cord; our body's primary control center for processing information, coordinating behavior, and maintaining homeostasis (balance in our body)
Peripheral nervous system (PNS) which is made up of our nerves outside the brain and spinal cord, acting as a communication network between the central nervous system (CNS) and the body's muscles, organs, and skin.
Our PNS is made of then 2 parts the Somatic Nervous System (SNS) (the side we control our muscles and movement, think voluntary control) and Autonomic Nervous System (ANS) (the side that is involuntary control: Sympathetic and Parasympathetic)
The sympatric and parasympathetics of the ANS require homeostasis or balance for us to be functionally well. We often break this down into parts of a “Fight or Flight” as the sympatheics and “Rest, Relax and Recover" as our parasympathetics. When these two sides are not in a balance with each other, that can “throw off” the ANS and impact how our body perceives pain.
Things that can push you more into the sympathetic side such as poor sleep, high stress, workload balance, postpartum changes, and training load levels, can all impact how that ANS is functioning.
Any pain, and in this case, back pain can be directly influenced by what is going on in the ANS and how “on edge” the system is acting.
Back to the Back Pain:
If someone is in pain, or they strained their back, many times our body will go into a protection mode. The muscles surrounding the area of the perceived pain, tighten to guard the area and protect it. Over time, that area can then have increased sensitivity, meaning, it doesn't take as much influence of perceived injury to the area, to elicit the pain response. Then the brain starts to change how and what you are doing, to reduce the chance of it starting to hurt. We then all of a sudden can’t bend forward without feeling some type of pain.
When this cycle continues for longer periods of time without resolving, we then become more influenced by certain factors. While the back may have started out as the problem spot, it may not actually be the back that is the problem, but its responding to the environment around it.
Examples of this can be the way you are sitting at your desk, while you are stressed with a work deadline; the influence of postpartum mom, who is also now having to lift and carry 10lbs throughout her day; starting a new workout routine and sleeping poorly.
So the treatment for treating the pain is not just about the muscles in the area of the perceived pain, but also treating the whole nervous system.
Dry needling for pain
Dry needling does work at a local level. We know this from studies that show when inserting the needle into a trigger point, you can get a local twitch response, we get increased blood flow to the area, and muscle tone can be reduced in that area, which can be contributing to the local pain. But this is only a part of the effects of the dry needles.
Dry needling also impacts the Autonomic system, allowing for changes in the processing of the pain. The effects of the dry needles on the parasympathetic side of the nervous system causes the body to shift out of that “fight or flight” mode, into more of the calming/relaxing side. This is why people will sometimes report feeling calm, relaxed or sleepy post dry needling sessions. When this is happening, the body is shifting out of that protective mode, contributing to less guarding and less pain sensation. When our body is not feeling guarded or in pain, we have the ability to actually move better. Moving better is actually a key component to getting out of pain, because you are teaching the body that it is safe to move, and the response to stop the movement is diminished. When our bodies perceive the feeling of safety with movements, the alarm bells of pain are quieter.
This is ultimately what leads to feeling less pain post dry needling, and actually feeling better.
Why Exercise Still Matters Most
While quieting the pain sensation is an important part of moving better, dry needling alone is usually not enough. Dry needling isn’t about “fixing” your back, it’s a tool to help you move with less discomfort so you can get back to the strength and mobility work that actually drives long-term change in our bodies, allowing your body to adapt itself. Dry needling needs to be paired with strength training, mobility work, and load management in order for the body to truly recover function. Dry needling with exercise is how you start to feel better, but then also start to move better so the pain does not come back. Exercise also is acting on the nervous system, retracing the brain and nervous system that it is safe.
So that person that comes in feeling better after 2-3 sessions isn’t typically done in their rehab journey. The good thing is the pain is usually no longer the barrier to actually moving. The movement and exercise is what we know actually will help them stay better and help keep their body more resilient in the long term.
It’s Bigger Than the Needle
Dry needling is so much more than releasing a tight muscle. It's impacting an entire nervous system that is influencing that muscle. When we have pain, it does not mean our bodies are broken, it just means our bodies are adaptable to the influences on it. When we can change how the system responds, we can change how our bodies can move.
And because our pain is multifactorial, treating pain just at a local level will help, but doesn’t change the pain in the long term.
References:
Bialosky JE, Kearns WD, George SZ.
Dry Needling and Acupuncture for Musculoskeletal Pain: Mechanisms and Clinical Implications.
Physical Therapy Reviews. 2010;15(4):263–267.
Dommerholt J.
Dry Needling — Peripheral and Central Considerations.
Journal of Manual & Manipulative Therapy. 2011;19(4):223–227.
Langevin HM, Churchill DL, Cipolla MJ.
Mechanical Signaling Through Connective Tissue: A Mechanism for the Therapeutic Effect of Acupuncture.
FASEB Journal. 2001;15(12):2275–2282.
Dunning J, Butts R, Mourad F, et al.
Dry Needling: A Literature Review with Implications for Clinical Practice Guidelines.
Physical Therapy Reviews. 2014;19(4):252–265.
Fernández-de-Las-Peñas C, Nijs J.
Trigger Point Dry Needling for the Treatment of Myofascial Pain Syndrome: Current Perspectives Within a Pain Neuroscience Paradigm.
Journal of Pain Research. 2019;12:1899–1911
Boyles R, Fowler R, Ramsey D, Burrows E.
Effectiveness of Trigger Point Dry Needling for Multiple Body Regions: A Systematic Review.
Journal of Manual & Manipulative Therapy. 2015;23(5):276–293.
Cagnie B, Dewitte V, Barbe T, et al.
Physiologic Effects of Dry Needling.
Current Pain and Headache Reports. 2013;17(8):348.
Kietrys DM, Palombaro KM, Azzaretto E, et al.
Effectiveness of Dry Needling for Upper-Quarter Myofascial Pain: A Systematic Review and Meta-analysis.
Journal of Orthopaedic & Sports Physical Therapy. 2013;43(9):620–634.
Shah JP, Thaker N, Heimur J, et al.
Myofascial Trigger Points Then and Now: A Historical and Scientific Perspective.
PM&R. 2015;7(7):746–761.
Perreault T, Fernández-de-Las-Peñas C, Plaza-Manzano G, et al.
Dry Needling in Physical Therapy Treatment of Chronic Pain: Systematic Review.
Journal of Clinical Medicine. 2024;13(4):1123.
What is my Nervous System and what are the parts?
The nervous system is a complex network of nerve cells and fibers that transmit signals between different parts of the body. It is responsible for coordinating actions and responses by processing sensory information, regulating bodily functions, and facilitating communication between the brain and spinal cord with the rest of the body. Comprised of two main components, the central nervous system (CNS) and peripheral nervous system (PNS), it plays a crucial role in everything from voluntary movements to involuntary processes like heart rate and digestion. The nervous system allows humans to react to their environment, control movements, and maintain homeostasis, making it essential for overall health and well-being.
The central nervous system (CNS) and peripheral nervous system (PNS) serve distinct but interconnected roles in the body. The CNS, consisting of the brain and spinal cord, is responsible for processing and integrating sensory information, controlling motor functions, and coordinating complex thoughts and behaviors. In contrast, the PNS encompasses all the nerves outside the CNS, including sensory and motor nerves that extend to limbs and organs, facilitating communication between the body and the central nervous system. While the CNS acts as the command center, the PNS functions as a network that relays messages to and from the periphery, ensuring the body responds appropriately to stimuli.
The peripheral nervous system (PNS) is a crucial component of the nervous system that connects the central nervous system (CNS) to the limbs and organs. The PNS can be further divided into the somatic nervous system, which controls voluntary movements and sensory information, and the autonomic nervous system, responsible for involuntary functions such as heart rate and digestion. Within the autonomic system, there are two branches: the sympathetic and parasympathetic nervous systems, which work in tandem to manage the body's responses to stress and recovery. Understanding the PNS is vital for recognizing how physical activity, rehabilitation, and overall wellness impact body function and mobility.
The autonomic nervous system (ANS) is divided into two main branches: the sympathetic and parasympathetic systems, each playing distinct roles in regulating bodily functions. The sympathetic system prepares the body for "fight or flight" responses during stressful situations, increasing heart rate, dilating airways, and releasing adrenaline to enhance alertness and energy levels. In contrast, the parasympathetic system is responsible for the "rest and digest" functions, promoting relaxation, reducing heart rate, and facilitating digestion and recovery when the body is in a calm state. Together, these systems maintain homeostasis by balancing the body’s reactions to external stimuli and internal needs.
When we experience pain, our autonomic nervous system (ANS) often leans more towards sympathetic activation, triggering the “fight or flight” response. This shift prepares the body to react quickly to perceived threats, leading to increased heart rate, heightened alertness, and muscle tension. In this state, the body prioritizes immediate survival over other functions, which can hinder healing and recovery. Chronic pain can perpetuate this sympathetic dominance, creating a cycle that not only intensifies the sensation of pain but also impacts overall well-being. Addressing this imbalance through targeted physical therapy can help restore homeostasis and promote a more calming parasympathetic response, facilitating recovery and improved quality of life.
At Mobilitide Physical Therapy, we recognize that a comprehensive approach to healing involves not just the musculoskeletal system, but also the nervous system, which plays a crucial role in pain perception and overall quality of life. We are trained to incorporate techniques that address both physical and neurological aspects of recovery, ensuring that our clients experience not only relief from pain but also enhanced mobility and function. By understanding the intricate connections between the nervous system and musculoskeletal health, we create individualized treatment plans that promote long-term wellness and empower clients to engage fully in their daily lives.